COSHH is the law that requires employers to control substances that are hazardous to health.
This detailed guide includes a definition of COSHH, a summary of what’s covered by COSHH, explanation of important symbols, details of how to create a COSHH assessment, common mistakes and a compilation of latest articles on the subject.
- DOWNLOAD: Factsheet on chemicals and COSHH
- Handing hazardous substances – top tips
- Health & Safety Executive’s essential guide to COSHH
- Chemical safety data sheets
- Take RoSPA’s ‘What is COSHH?’ quiz
- Barbour EHS COSHH/Hazardous Substances guide
Harmful substances video
COSHH stands for the Control of Substances Hazardous to Health.
These regulations, created in 1999 and amended in 2002 to include EU directives, require employers to control exposure to hazardous substances to prevent ill health.
 Hazardous substances include:
Hazardous substances include:
- chemicals
- products containing chemicals
- fumes
- dusts
- vapours
- mists
- nanotechnology
- gases and asphyxiating gases
- biological agents
- Germs that cause diseases
It does not cover asbestos, lead or radioactive substances.
Essential COSHH symbols
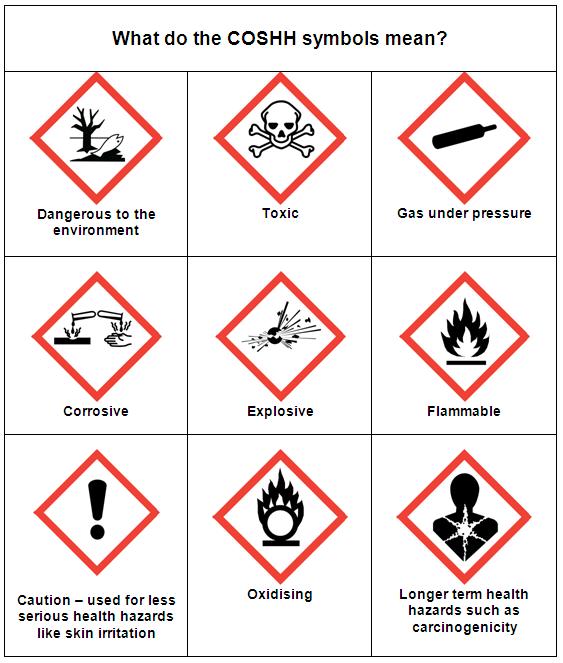

Preventing exposure
 You can prevent or reduce workers exposure to hazardous substances by:
You can prevent or reduce workers exposure to hazardous substances by:
- Discover the health hazards
- Risk assessment (templates from HSE here)
- Control measures to reduce harm
- Provide information and training for employees
- Monitoring health
- Plan for emergencies
Most businesses use substances, or products that are mixtures of substances.
Some processes create substances. These could cause harm to employees, contractors and other people.
Sometimes substances are easily recognised as harmful. Common substances such as paint, bleach or dust from natural materials may also be harmful.
30 minute video explaining COSHH
7 steps of COSHH
This infographic by Abacus Safety explains seven steps practitioners can take.

How to create a COSHH assessment
Check out this useful video by Sevron Safety Solutions on creating assessments and complying:
Five common COSHH mistakes from Phil Chambers BSc CMIOSH
 Over the years, I have seen a range of assessments of substances hazardous to health. Some pose problems, so here are five common mistakes and what you need to do to avoid them.
Over the years, I have seen a range of assessments of substances hazardous to health. Some pose problems, so here are five common mistakes and what you need to do to avoid them.
Mistake 1: A collection of datasheets
I sometimes go into companies and the management says: “Here’s our COSHH file.” You look at it and find that it is just a collection of (often incomplete) datasheets.
What you are required to do is assess the risks from each substance depending upon how you use it in your workplace, then put appropriate measures in place to control the risk.
Finally, you have to verify that those control measures work. And don’t just go by what you’ve bought recently; open up cupboards and see what might be lurking.
Mistake 2: A perfect set of COSHH assessments sitting on the shelf
The next mistake is to have a perfect set of COSHH assessments in a pristine folder, while people on the shop floor don’t know anything about them.
A thick manual full of assessments and datasheets on the shop floor is not a workable solution, so I promote the practice of having summaries at the point of use.
These state how the substances are to be used and the emergency measures to take in the event of an incident. You also have to talk to people about these instructions.
It is best practice to involve them when coming up with the control measures in the first place — that way they are more likely to buy into them.
Mistake 3: Getting distracted by trivia
I have seen control measures for a carcinogen lost in a collection that included Mr Sheen (with separate assessments for Original and Pot Pourri).
If you assess every substance on your site, then apart from the effort involved, you will end up with an unworkable system where the critical substances are masked by t he trivial ones.
he trivial ones.
It is critical that people using substances believe that following the control measures is a necessity. If they are asked to follow measures that they regard as silly, it can devalue the whole approach.
By all means cover yourself by listing substances that are low risk, but don’t clog up the main system.
Another way of making it controllable is to group substances together. For example, printing inks for a particular type of printing process are generally the same, irrespective of their colour.
So just have one assessment for conventional litho inks, another for digital inks. Don’t have one for magenta, one for cyan, etc.
Mistake 4: Failure to follow the hierarchy of control measures
There is a hierarchy of control measures you need to follow, with elimination/substitution at the top of the list and PPE at the bottom. Often, people put effort into the middle and lower order control measures and never consider substitution.
Where a substance is an inherent part of your process, substitution may be unrealistic.
But there are plenty of solvents and cleaning substances in use where less hazardous alternatives are available.
To aid management commitment, I use a colour coding system of:
- green – no effect
- amber — short-term effect, such as solvents which cause light-headedness on inhalation over-exposure
- red — medium/long term effect such as corrosive substances which burn the skin or cause permanent eye damage
- purple — long term effects such as carcinogens.Once you have a colour code, agree a policy of working towards the green end of the colour coding, starting by attempting to remove purple substances, with KPIs of how many of each colour have been removed.
Mistake 5: unrealistic use of personal protective equipment (PPE)
People on the shop floor need to “buy into” the practices around hazardous substances. One good way of defeating this is to require staff to wear PPE for everything.
A substance may irritate to the eyes, but so is soap, and you don’t wear goggles when you wash your face. You want to make sure that people wear eye protection when handling a substance that has a serious risk of eye damage.
Datasheets tend to recommend PPE, even when there is no effect. What the supplier has to address in his datasheet is all possible uses of the substance.
Assess the outcome based on what you do and take appropriate steps. The two may not be the same and your PPE requirements need to suit the latter.
With all risk control measures, the emphasis should be on effectiveness and implementation. If you avoid the above pitfalls, you can be well on the road to achieving good control of substances hazardous to health in your workplace.
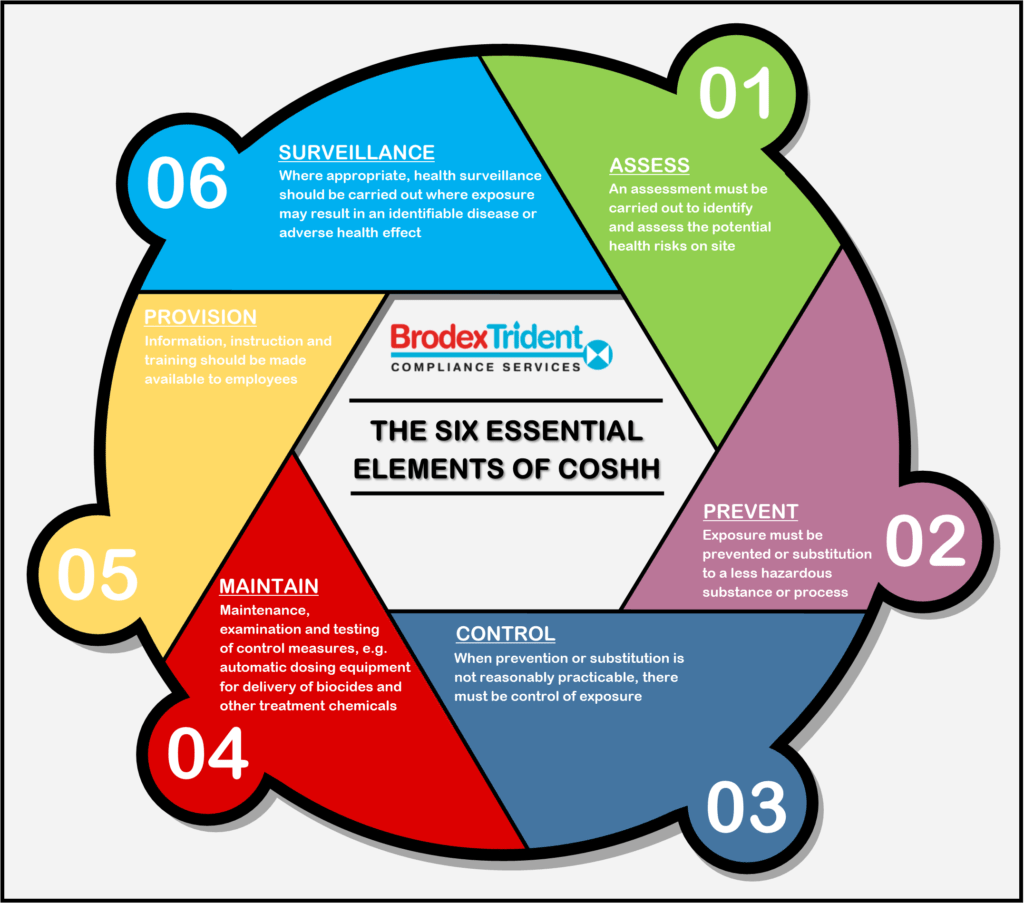
The six essential elements of COSHH
History of COSHH
Dr Adrian Hirst talks to industry experts about how COSHH has improved occupational health and what further action is needed.
COSHH is such an integral part of the way in which exposure to hazardous substances in the workplace is approached today, that one may wonder what it was like prior to 1989.
 Martin Stear, co-director of WES, an an independent occupational hygiene consultancy and registrar of the BOHS’s faculty of occupational hygiene:
Martin Stear, co-director of WES, an an independent occupational hygiene consultancy and registrar of the BOHS’s faculty of occupational hygiene:
“Employers still had to complete assessments under the Health and Safety at Work etc Act 1974 (HSWA) and the Factories Act 1961.
“It would be wrong to suggest that industry wasn’t doing much but COSHH gave a greater emphasis to hazardous substances and got employers to focus better on what was already implicit in law.”
Lynne Morgan, CEO of El Morgan, notes that the same hierarchy of control was being used for every type of occupational hygiene survey and audit:
“We just weren’t doing formalised, full written risk assessments.”
 Tracey Boyle, co-director at WES, COSHH’s arrival in 1989 was “a wake-up call” for the industry.
Tracey Boyle, co-director at WES, COSHH’s arrival in 1989 was “a wake-up call” for the industry.
“There was a lot of interest. COSHH was widely publicised and seen as the biggest thing since the HSWA.
“Unions were very excited about the legislation.
“People in industry had concerns about how the new laws should be managed by employers and how they would be enforced.”
 Andy Gillies, managing director of Gillies Associates Ltd, and from Dow Chemical Company, where his role specifically created due to a perceived need for in-house knowledge to successfully implement COSHH:
Andy Gillies, managing director of Gillies Associates Ltd, and from Dow Chemical Company, where his role specifically created due to a perceived need for in-house knowledge to successfully implement COSHH:
“Within the Dow Chemical Company, the introduction of COSHH was taken very seriously. We all knew what was coming and what was needed. Organisations were striving for an efficient way to implement the regulations — especially with regard to risk assessment, training and records.
“Risk assessment was a cornerstone of COSHH right from the beginning, however, we built on work that had already been done.”
Looking at the major developments in the COSHH regime over the last 25 years, one change which is often highlighted is the introduction of control banding — a technique used to guide the assessment and management of workplace risks.
In 1998, BOHS published a series of papers central to the early development of the control banding approach in The Annals of Occupational Hygiene; of course, control banding is now widely applied in the COSHH Essentials regime as well as other control banding approaches used worldwide.
Commenting on the approach, Mr Gillies says: “In the early days of COSHH people were overwhelmed by the huge numbers of substances. With the introduction of control banding, people realised that banding substances could be a manageable way of dealing with many different substances.
“Today, we see control banding being used in quite a large range of settings, including the pharmaceuticals industry, fine chemicals and the speciality chemicals sector. It can be very useful, although it can also be misapplied, so needs care in its use.”
Carcinogens Directive
Another welcome development, as far as many occupational hygienists were concerned, related to the amendments to COSHH made in order to implement the Carcinogens Directive in the UK.
In particular, it was felt that the actual listing of known carcinogens, in schedule 1 to COSHH, was invaluable in spelling out the status of certain substances as dangerous carcinogens and thereby improving the control of exposures to carcinogens under the COSHH regime.
Other major changes included the replacement of maximum exposure limits and occupational exposure standards with workplace exposure limits and the introduction of the principles of good practice as set out in schedule 2A. Both of these changes were contained in the COSHH Regulations 2002, as amended, which came into force in 2005.
The change in emphasis achieved by the advent of schedule 2A to COSHH in listing the eight principles of good control practice, was important in terms of evaluating the controls rather than emphasising exposure limits alone, notes Ms Boyle.
“In a practical workplace situation, it is easier for inspectors to see if people are complying with the eight principles of good control practice than to focus on air sampling values,” she says. “The changes also helped in listing exactly what good control should look like.”
This view is echoed by Mr Stear who says that he often refers employers to the eight principles of good control practice when suggesting changes for workplaces, rather than focusing purely upon exposure limits.
In response to a question about what COSHH has achieved in the last 25 years, a spokesperson at the Health and Safety Executive (HSE) said: “HSE statistics indicate that work-related ill-health cases have generally reduced over the last 10 years, although given the high numbers involved more can and still needs to be done to make further improvements.”
Mr Gillies says of the legislation:
“COSHH has been an important driver in improving standards in occupational health. If COSHH weren’t there, there’d be far less incentive to make improvements.”
In the same vein, Ms Boyle is of the opinion that COSHH has raised awareness of hazardous substances at work, although she still thinks that a lot of work remains to be done. “Before COSHH, people tended to be focused on highly hazardous substances like asbestos and lead and it was fairly difficult to enforce control of other hazardous substances,” she says.
“The HSWA was all implicit and the good thing about COSHH is that the regulations made the control of hazardous substances explicit. It also covered all hazardous substances rather than the specific ones like lead, asbestos and so on. It really made people think about what they were using at work or in their business.”
Despite this progress, a number of occupational hygienists believe that there remains a small and large company divide with regard to what COSHH has achieved. In the case of large companies, even 25 years ago, good work was being carried out with regard to the management of risks associated with hazardous substances.
However, there are concerns about smaller companies that have to deal with hazardous substances, which is why initiatives like HSE’s COSHH Essentials guidance and tailored COSHH support on the HSE website for smaller companies, such as hairdressers, beauticians, caterers and bakeries are so welcomed.
Mr Gillies warns: “Even now, 25 years later, some companies still don’t know about COSHH and there is a lack of understanding with regards to the basics — such as risk assessments. Companies may think they need to generate lots of paperwork rather than focusing on making the risk assessment practical and relevant.”
After a quarter of century, one would hope that the COSHH regime would be working smoothly. However, occupational hygienists continue to report a lack of understanding in terms of its basic principles, highlighting an ongoing need for a greater grasp of the regulations.
Niall Evans, managing director of Epsilon Training and Consultancy Ltd and a former HSE principal specialist inspector, says: “Many people and companies struggle to understand the requirements of the regulations, seeing them as an exercise in simply recording the substances that are used. They often include chemicals that are not hazardous to health and some that present no other hazards, such as flammability. For most, deciding the level of risk and the appropriate controls is a headache. Many of course rely too heavily on personal protective equipment.”
Ms Boyle, another former HSE inspector, would like to see something explicit in COSHH in future, specifying the use of qualified occupational hygienists for situations that demand such expertise.
“Sometimes you see poor advice being given by people who are not competent,” she says. “The employer then spends a lot of money on the basis of that advice, for example, building a particular local exhaust ventilation system that will never work. I’ve seen hundreds of thousands of pounds spent on systems that will not control exposure, as well as shocking reports from people who are not competent to advise on occupational hygiene matters.”
BOHS’ president Mike Slater believes there is a pressing need for better enforcement of the COSHH legislation in future, arguing that research has indicated that compliance with some elements of COSHH makes for shocking reading.
“In Dr Lesley Rushton’s research, compliance in the case of workplace silica exposures was estimated at just 33 per cent,” he concludes.
“The COSHH regime can only be as strong as its weakest link and we believe that robust enforcement to improve compliance by employers is vital to the future success of COSHH.”























When with the HSE I called upon a Demo job with a Major Stake Holder. (Drug Manufacturer) Nosing about, I came accross brown jars with yellow Skull & Crossbone warning markers on them, about 20, 5 litre containers. They were neatly placed within a room due to be demolished. Adjacent walls were alreading knocked down on the concrete floor, along with huge steel doors. (An indication perhaps of the severe nature of chemiclals housed within?) When I enquired why they were still present, I was informed by the Site Agent and Foreman that they were empty? And when I asked… Read more »
And don’t forget chemicals react and you may not have an off the shelf SDS for the reaction product which could propose different hazards to the original materials. (Example: silica solid + hydrofluoric acid aqueous soln gives off Silicon trtraflouride. Toxic gas)
I completely agree. I have seem much of the same. Refreshing to see it written down
The summary at point of use is a good idea. Also the points on PPE over use are well made.
A really good piece Phil, written plainly and succinctly and useful to Line Managers and Supervisors.
A great article Phil. Colour coding is an excellent idea.
I agree entirely with the focus on medium to high risks but still pull my hair out at the idea of writing pages of information (that no-one will bother to read) about such things as Fairy Liquid!
Whilst it is clear that there ius still (after all these years) confusion surrounding COSHH, just how much will there be when REACH asks everyone to dublicate (in spades), what we have already done since 1988, thanks to Bureaucratic EU Overkill??
In the words of the fa,ous American: “You ain`t seen nothin` yet!”
Still, crats, wherever they are employed never learn “Easy or Uncomplicated”!
Sue from Looe – The company I work for also require MSDS’s to be no more than three years old. I worked at a new site that we took over where a large number of the MSDS’s were dated in the 1990’s. In a lot of these data sheets there was one common factor being that the first aid instructions said to induce vomiting if swallowed, whereas now this is recognised as being very dangerous as the substance can do just as much damage on the way back up as it did on the way down. If you notice now,… Read more »
Pertinent points made in the article – nicely done.
People do seem to make heavy weather of COSHH, with a fear of “Chemicals” rather that a consideration of hazards and controls. Too often the assessment is little more than an antiquated collection of SDSs. I prefer a (where appropriate) a process or operational approach rather than a substance by substance battle against the odds.
Very useful information with a sensible usable approach.
Excellent summary. I particularly like the colour-coding idea. The variable quality of SDS, confusion with COSHH and who they are written for was discussed at a meeting I attended yesterday
Good aticle, sensible and practicle. I also like the colour coding idea, visual aids usually help.
Please don’t dismiss Oxygen. (after all you’d consider oxidising agents?) The old trick of welders (oxy-acetylene) working in enclosed areas, sweetwening the air by venting oxygen can be disasterous. Consider every substance and ask – can it cause significant hazard, – is that hazard likely to occur – only if yes to both then document and mitigate.
Thanks for the comments, guys. Very much appreciated. Like the comment on reaction products. Hydrofluoric acid itself is one of the worst substances with which I have had to work. See http://www.ab.ust.hk/hseo/tips/ch/ch005.htm for the fatality in Western Australia; poor sod took 15 days to die. (I was working with HF in Melbourne at the time.)
An excellent passage. All too often I have experienced the same problem from employers / clients where they think that COSHH assessments are the data sheets. To anyone with limited knowledge of COSHH this is an educational piece of information. It is amazing that here we are in 2014 and the original legislation came into force in 1988 with many still not sure what COSHH is about.
It is good advice when you are in control of your own processes, people and environment. Many of us though are constrained by the requirements of a client when on their site. They often have a ‘no common sense’ approach and therefore expect us to have one! PPE for everything, substituting over the top controls for short term work ,(I have been told to use fixed scaffold for a 10 minute job..honest!, the reason being, “if it can be done, it should be done.”) I have had to produce CoSHH assessments for oxygen..! (Seriously..) Those of us with more enlightened… Read more »
very informative, and common sense approach.
Excellent article. I’m working towards all of the best pracise in this piece, and particulary like the colour coding but I’ve been asked by my HSE Director to make sure all SDS’s we are holding are no older than 3 years. This is difficult as checking suppliers websites, their SDSs can be 5 years old or older. We hold mineral oils whcih are not re-ordered often so the correesponding SDS is the same age as the substance. I think this is right – it mateches what we have. Later versions of SDSs for the product may not reflect excatly what… Read more »