By Sara Brown, Deputy Chief Officer for Workforce Development, Birmingham Children’s Hospital
Carers in any sector – in healthcare, in voluntary work – are known to be more at risk of serious stress-related and psychological problems. They take troubles onto their shoulders and don’t always know when to stop. As opposed to ‘burnout’, the gradual build-up of stress, worries and a feeling of overwork over time, ‘compassion fatigue’ can also lead to a sudden crisis with few obvious warning signs.
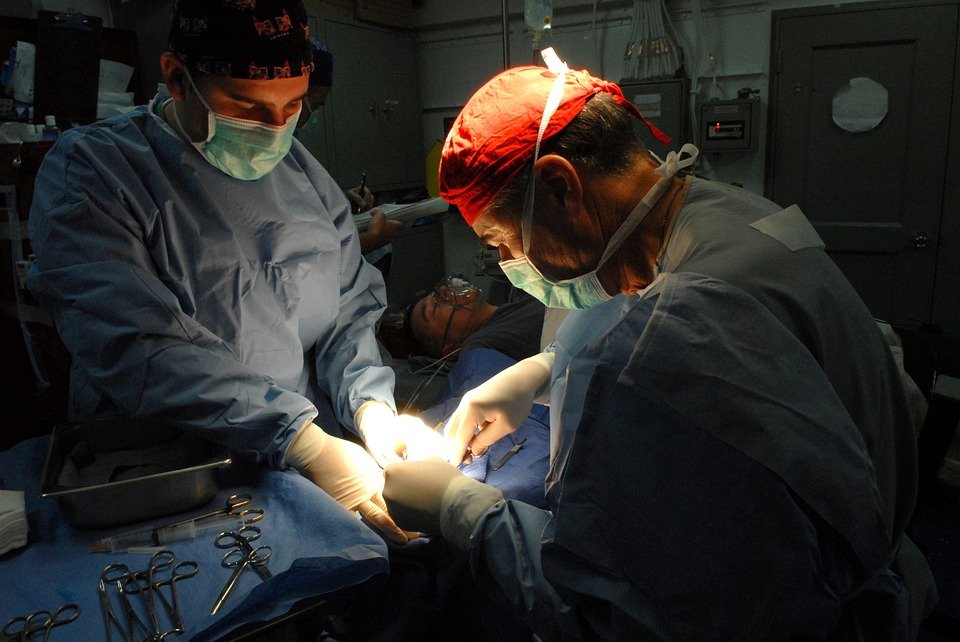
Birmingham Children’s Hospital is one of the UK’s leading providers of paediatric care, treating and supporting 90,000 children, young people and their families each year. The hospital has a global reputation for specialist services, including the treatment of the most complex heart conditions, chronic liver and kidney disease, cancer, serious burns, epilepsy, neurology and cystic fibrosis. It’s also home to Europe’s largest single-site intensive care unit for children, a major trauma centre and mental health services.
The facilities and technical expertise are world-leading, but it’s the hospital’s team of 3,700 people that work on behalf of the children and their families, who provide the all-important human touch, care and support. Working with often seriously ill children can, understandably, have an impact on employees, many of whom deal with sensitive and emotional situations on a daily basis, having conversations about end-of-life care or coping with the consequences of incidents and trauma. We know that resilient and happy teams are able to offer the best possible care. Our teams make a real difference to the experience of our patients and their loved ones. They provide the x-factor in the treatment.
Looking closely at the findings from the National Staff Survey there was evidence of a rising number of people experiencing stress relating to work. While employees were admitting to suffering from stress, actual sickness absence rates at the hospital continued to be low (running at levels just above 3%, compared with 4% in the NHS nationally), suggesting that committed employees were fighting through their issues, while also potentially bottling up the stress. We had an external counselling service in place for staff. But we found we needed something more responsive and flexible to inspire total confidence and trust.
In 2014 we put together a revamped package of health and wellbeing activities to cover the basics of sleep, diet and exercise, alongside training for senior nurses and managers around stress awareness and the opportunity to learn new skills such as mindfulness. An integral part of the improved staff offering was a new counselling service that offered a 24/7 expert telephone support service and face-to-face counselling.
Working with a new psychological wellbeing specialist in CiC meant we knew we had a full service in place. Any employee can contact the telephone service for a confidential discussion with a trained counsellor. The issue is worked through in conversations, or can be ‘triaged’, with the employee referred on for off-site, face-to-face counselling. Under the new service no-one has to wait more than a week for an appointment, and usually no more than two days. The hospital worked with CiC on a specific comms and marketing strategy to raise awareness of the service and ensure uptake of the service, trying to help make talking to the service a ’normal’ option with no stigma attached. This included the standard leaflet and intranet material for existing staff, as well as promotion through our staff induction programmes and materials around our hospital where employees might go when they need time to themselves.
Any employee can contact the telephone service for a confidential discussion with a trained counsellor. The issue is worked through in conversations or can be ‘triaged’, with the employee referred on for face-to-face counselling. Counselling is always provided off-site in order for people to feel confident that confidentiality is assured and they are free from immediate work pressures. The service is tailored, meaning a counsellor is matched to employee needs and located within at most 15 miles from the hospital or home. No-one waits more than a week for an appointment. In fact, it’s usually no more than two days.
Most important was the level of responsiveness and flexibility we’ve seen from CiC. We have to be certain our employees get the right response when they need it. We’ve found the same attitude in our requests for updates and reporting. They have come in to deliver briefings when we have asked and have been responsive to our needs. CiC also provides an additional service for line managers, providing advice and guidance on how they can best identify and support their staff who are struggling with stress.
What we’ve learnt is that it’s possible to build an approach based on open and on-going conversations about the impact of stress, that provides more of a sense of security and support. We also know that our nurses and managers have an important part to play in spotting signs of issues and encouraging the honesty that’s needed. Staff under pressure have found an important outlet for talking about and dealing with their challenges. Since 2013 our staff surveys have shown a pleasing reduction in the numbers of our employees experiencing work-related stress.
In the period from 1 November 2014 to the end October 2015, 11% of our employees had used the CiC service at some stage. Commonly, the conversations related to dealing with raised levels of pressure and problems with relationships (which could be at work or home). 44% of people who accessed the telephone service went on to take the opportunity available for face-to-face counselling. We’re pleased to see good levels of use of the service. We encourage a culture of openness here – it’s all part of our sense of being part of a community. If there’s a problem, people come forward and we tackle it constructively. We have to be realistic and understand that in a working environment like ours stress will occur.
Our children and families do not expect or want our nurses to be smiling robots. What’s needed, though, is confidence. Confidence that any of us, at whatever level in the organisation, can talk about how we’re feeling; that there’s no stigma; that there are right systems being run by the right people all in place to help.
The next development we’re looking at is the need for more specific advice. The counselling was originally commissioned to focus on tackling work-related stress rather than provide the more general advice that an Employee Assistance Programme offers. But we now want to explore whether there are other sources of stress we might be able to support staff to deal with, such as financial worries.
Sara Brown is the Deputy Chief Officer for Workforce Development, Birmingham Children’s Hospital
What makes us susceptible to burnout?
In this episode of the Safety & Health Podcast, ‘Burnout, stress and being human’, Heather Beach is joined by Stacy Thomson to discuss burnout, perfectionism and how to deal with burnout as an individual, as management and as an organisation.
We provide an insight on how to tackle burnout and why mental health is such a taboo subject, particularly in the workplace.